This series of papers proposes solutions to American governmental problems that could be addressed by a Constitutional Convention. Please refer to American Rebirth Paper No. 0 to understand additional context of this paper and subsequent papers. American Rebirth Paper No. 6 addressed problems with the Federal budget and proposed solutions to alleviate those problems. As stated in American Rebirth Paper No. 6, it is proposed that the Social Security and Medicare programs be eliminated. American Rebirth Paper No. 7 addressed Social Security. This Paper No. 8 will address Medicare and other Federal health programs.
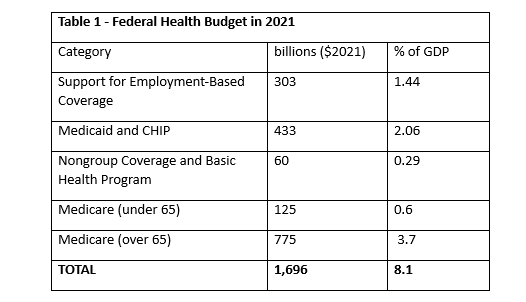
The total budget (expressed as a percentage of the GDP) in 2021 for Medicare, Medicaid, and other Federal health programs is shown in Table 1:
For people under 65, the federal government subsidizes health insurance in several ways:
By giving tax benefits for employment-based coverage.
By providing a majority of funding for Medicaid and the Children’s Health Insurance Program (CHIP) (states provide the remainder).
By offering tax credits to eligible people who purchase coverage through the health insurance marketplaces established by the Affordable Care Act (ACA).
The federal government also provides coverage through the Medicare program to people under 65 who receive benefits from the Social Security Disability Insurance program or who have been diagnosed with end-stage renal disease.
Medicare and Medicaid are funded through payroll taxes (34% of total funding), the General Fund of the Federal Government (47%), premiums paid by retirees enrolled in Medicare (15%), and 4 percent from other sources. Those of you currently working and paying payroll taxes might believe that you are funding future health insurance that will be provided by Medicare with no cost to you. This is not the case. Not only will you need to pay a premium for Medicare (unless you have no income other than Social Security), you will likely want to purchase supplemental insurance to provide additional insurance because Medicare only covers about 80% of the typical healthcare costs seniors face—leaving a few significant gaps in coverage. Medicare Supplement (Medigap) plans are policies designed to help extend coverage, lessen costs, and ultimately give beneficiaries peace of mind at all times.
Table 2 shows historical health care spending per capita in the United States from 1960 (before Medicare and Medicaid) through 2019. Costs per person are shown for the actual year and in dollars adjusted for inflation (expressed as $2012).
With a population of 329 million in 2019, the total health care spending in 2019 was $3.8 trillion. Of this amount, 43 percent was government spending and 57 percent was private spending, which is primarily health care coverage that is provided by employers for their employees.
Why are we spending over nine times more per person in 2019 for health care relative to 1960? Part of the increased cost is due to advances in medical treatment. These medical advances have increased life expectancy, from 70 years old in 1960 to 79 years old in 2019. A doctor in 1960 may have been unable to do anything for a patient sick with a serious illness, but a doctor in 2019 may be able to treat the same illness. Because the doctor in 2019 is treating the patient, the treatment cost for this hypothetical illness obviously is greater.
Medical advances include improvements in cancer treatment. Someone that was diagnosed with cancer in 1960 may have had very few treatment options while in 2019 most cancers are treatable. For example, the death rate (per 100,000 population) for breast cancer in 1960 was 32; by 2019, the death rate for breast cancer has been reduced to 20. A similar trend has occurred for colon cancer. The colon cancer death rate in 1960 for men was 33, and by 2019 the death rate had been reduced to 16. Not only has treatment improved, but early diagnosis, such as with mammograms, and preventative measures, such as routine colonoscopies to remove pre-cancerous polyps from colons, have allowed cancers to be treated early before the cancer has become widespread, thus improving the success rate of treatment.
While our health care system can do more with diagnoses and treatment, that does not explain all the increased cost. Some of the increase is due to increased administrative costs, primarily due to more regulations, which inevitably require copious amounts of paperwork. Our health care system is extremely complex due to regulations. These regulations open the door to fraud, which costs the taxpayers billions of dollars per year. Something as simple as providing free care to someone who comes to an emergency room and says they have no insurance and no means to pay for the care, is made difficult due to regulations. The hospital simply cannot provide free care, no questions asked; they must attempt to make the patient pay due to Medicaid regulations. As a result, the hospital spends time and budget on paperwork that they know is pointless.
In contrast to the increase in costs that are related to health care covered by private and public insurance, costs for medical procedures that are not covered by either private or public insurance have been decreasing. Two notable examples are elective plastic surgery and Lasik eye surgery. Both competition and technological advances have helped to lower costs. Once procedures and equipment are approved by the Food and Drug Administration (FDA) for use, doctors that perform these elective procedures are not encumbered by onerous regulations. If they provide quality services that are consistent with industry standards, they will be able to continue to provide services. As with any competitive industry, doctors will need to address any negative feedback they get from patients – too much public feedback that is negative will lead to loss of customers.
Technological advances have also occurred for procedures that are covered by insurance. These advances may be slower to market than for procedures that are not covered by insurance, but eventually new technology does make its way into the health care industry regardless of rather the procedure is covered by insurance. Given that technological advances should reduce costs, but health care costs are still increasing for insurance-covered health care, we can only conclude that regulations and too much involvement by the government in the health care system are the primary cause of increasing costs.
In my opinion, the following statements about our health care system are pertinent to any discussion regarding how to improve the system:
Regulations always increase cost.
Fixing prices rarely establishes a price that is spot on – either the price is too low or too high. If the price is too low, the availability of the procedure will be less than demand, resulting in shortages and long wait times to receive the service and/or rationing to limit the number of people who qualify for the procedure. If the price is too high, the excess payments go into the profits of insurance and health care companies – any excess is never rebated to the customer.
Free market competition naturally causes the price for a service to match demand.
Free market competition promotes innovation because innovation will create a competitive edge for whoever develops the innovation.
Free market competition provides an incentive to improve customer service. Comparing health care experiences where insurance-covered and government-regulated procedures are the primary service versus health care experiences for health care not covered by insurance, the experience in the latter case is generally better.
With our current health system, consumers usually have no understanding of the potential costs for a treatment, and they seldom shop around for a lower cost, but comparable procedure.
Payroll taxes for Medicare are simply taxes. They are not an investment in a future medical insurance program for you when you retire. Just like Social Security, Medicare is simply put a Ponzi scheme, where future coverage is dependent on future taxpayers.
Given a choice between spending money on health insurance and other uses for their income, many young, healthy individuals would rather not buy insurance.
There will always be low-income individuals and families that cannot afford to buy health insurance and have jobs that do not provide health insurance benefits. Since we are a charitable society, determining how we assist these individuals and families with health care is an important consideration.
Some individuals have pre-existing conditions, such as diabetes, that will require a known, and greater-than-average, health care cost.
Health care for end-of-life health care (such as for nursing homes) is typically the costliest expenditure in a person’s life.
Most health care providers are ready and willing to provide charitable services. In addition, for individuals without insurance that find themselves in an unexpected medical condition that will cause them to become bankrupt, the generosity of family, community, and fund-raising sites such as GoFundMe, will help to offset the costs.
An improved health care system would have the following features:
Maintain access to best-in the-world health care.
Reduce costs, particularly costs that are due to paperwork and other activities that are solely required by regulations.
Continue to promote innovation to improve treatment outcomes and reduce costs.
Individuals with pre-existing conditions need to be able to purchase insurance.
Reduce regulations.
Allow doctors to do what they do best – provide health care services for their patients. Reduce the amount of time doctors must devote to activities that do not involve patient contact and consultation.
Continue to aid individuals that cannot afford health care, even at the most basic level.
So, how do we use a Constitutional Convention to reform the government’s involvement in health care? First, we need to envision what is the best system, and then work from there. As you may have surmised from what I’ve written so far, I am an advocate of eliminating the Federal government’s involvement in health care, except for funding regulatory agencies, such as the FDA, and helping to fund research, including at the National Institute of Health (NIH) as well as at universities and other research facilities. This means eliminating Medicare, Medicaid, and Obamacare. This could be done by simply adding an amendment to the Constitution that states: “the Federal Government shall provide no funding to provide health care insurance to citizens or non-citizens of the United States, nor shall it provide funding to pay for health care. The Federal Government’s role in health care shall be limited to providing some funding (but not all) to support research into health care.”
Of course, by eliminating Medicare, Medicaid, and Obamacare, we have two important considerations to deal with:
What do we have to do to phase these programs out? Going “cold turkey” such that all the senior citizens on Medicare suddenly find out that they no longer will get any Medicare doesn’t seem fair, given that they have paid taxes their entire working career towards Medicare. So, at least for Medicare, some extension of benefits should be provided.
What is the best health care system, and how can the Federal Government help to support this system?
I will start by addressing the latter question. In my opinion, the best health care system can be achieved by doing the following:
Instead of paying payroll taxes into a government-run Medicare/Medicaid system, require workers to pay into health savings accounts (HSAs) at the same rate as the current Medicare taxes. The HSA accounts can be used to buy insurance (if not provided by the employer) or to cover deductible costs in the event of a high-cost health incident. (This aspect of the proposed approach will be expanded on following this list).
Require employers that provide health insurance to their employees to offer a high-deductible plan as an option to plans that have lower deductibles and more coverage. For the high-deductible plan, the employee will not have any required contribution (i.e. the plan is free to the employee). For all other plans, the employee must be required to contribute (i.e. have a monthly payment to help pay for the insurance) to the coverage.
For individuals and families that do not get insurance through an employer, which includes individuals that own their own business or do free-lance work as well as individuals that are employees, allow organizations to provide insurance through pooling of individuals and families. For example, the Dairy Farmers of American (DFA) is owned by and serves more than 13,000 dairy farmers in 47 states. The DFA could contract with an insurance carrier to provide insurance for their members. Members would pay a monthly premium to cover the cost. Typically, the insurance carrier will administer the insurance plan for a fee and all costs for medical will be borne by the organization. If the medical costs for a particular year are lower than average, the organization can either give rebates to its members or add the excess payments to a savings account that could be used for years where the medical costs are greater than average. As with employer-provided plans, plans provided by organizations must provide a high-deductible plan as an option. The high-deductible plan will have the lowest premium.
Eliminate all government regulations. Instead, provide government funding to third-party agencies that will establish best practices for medical procedures and health care. In addition, provide funding to third-party agencies that will conduct evaluations and reviews of health care establishments. The intent of this proposed approach to setting standards and quality control is not to force all health care organizations into identical approaches for health care, but to establish a standard that will become a benchmark for quality care. Healthcare organizations will be encouraged to develop procedures that exceed the current standard and will be asked to contribute to developing and improving on the standards. All government-funded agencies will be required to provide yearly reports to Congress, including any suggested improvements that could be made in best practices. Any suggested improvement must include a cost evaluation – if it costs twice as much to improve the health care, but the improvement is only a minor improvement, then it may not be worth establishing a new best practice.
All health care organizations must publish their all-in costs for specified procedures so that individuals are aware of potential costs prior to visiting the doctor or going ahead with a medical procedure. The goal with this requirement is to encourage individuals to compare prices from more than one provider before going ahead with a medical procedure. For example, for someone that has hurt his knee, the doctor may recommend an MRI. If the individual has a high-deductible plan, he will likely need to pay for the cost of the MRI. By knowing the cost, he can choose a health care facility that will minimize his cost.
For individuals with pre-existing conditions: if employed or a member of an organization that provides insurance, that individual is treated the same as all other employees or members. If the individual must purchase insurance on his own, he are placed into a pool along with others with pre-existing conditions. The pool of individuals is distributed to insurance companies based on the size of the company (e.g. a company with 10% of the market, will get 10% of the individuals). The insurance companies must allow these individuals to pay the same premium for insurance as individuals without pre-existing conditions.
Because Veterans often have special health care due to their involvement in military actions, the Federal government shall continue to provide health care for Veterans. This health care will be provided by health care organizations that are selected through a competitive process on a regional basis. For example, one region could cover Washington, Oregon, and Idaho. The contract agreed to by the Federal government and the health care organization would stipulate health care requirements that shall be provided by the organization and will establish metrics that will be used to measure the performance of the organization as required by the contract. If the organization under-performs on a metric, their payment will be reduced; if they out-perform on a metric, they will be paid a bonus. For example, the contract could stipulate that the health care organization track their performance in curing (or improving the lives) of Veterans with post-traumatic stress syndrome (PTSD). Third-party organizations funded by the Federal government will oversee establishment of best practices and will perform reviews and quality control assessments of the health care organizations. These contracts will be up for renewal every 10 years using a fully competitive procurement process. If an organization is obviously failing to perform, the government, at its sole discretion, can elect to start the contract renewal process in less than 10 years.
Provide basic health care services for poor individuals and families that cannot afford insurance. There’s a tough balance for these individuals. On the one hand, if free health care is provided that is on a par with health care that can be accessed by insurance, then there is a disincentive for individuals to purchase insurance – why buy insurance when you can get the health care for free? On the other hand, as a society we want to help those that are truly in need. The solution is to provide state-sponsored health care, but only to those that are truly in need, and require that those using the free health care be required to contribute a minimal amount to their health care. Such a system would have the following features:
a. Individuals and families must apply for access to the state-run health care system. Those that qualify will be given an insurance card that can be used at any state health care facility. Only those that have the state-issued insurance card can use the facilities.
b. Each state will own or lease health-care facilities, primarily walk-in clinics that can handle typical health issues, along with expensive diagnostic equipment (such as MRI machines). While the states will own the health-care facilities, private health care organizations will operate the facilities. The state shall hold a competitive process to procure the services of a health care organization; depending on the size of the state, multiple contracts could be issued on a regional basis. The lowest cost, qualified bidder will be awarded the contract. These contracts will be opened for competition every 10 years. If an organization is obviously failing to perform, the state, at its sole discretion, can elect to start the contract renewal process in less than 10 years. The state shall use an independent third-party to evaluate the performance of the health care organization per their contract requirements. For example, the contract could stipulate that average wait times at clinics shall be less than one hour; if average wait times are two hours, then the health care organization is not meeting the contract requirements. The health care organizations shall identify and recommend any capital improvements (for example, a new clinic or a new X-ray machine) that they believe will strengthen and improve the health care services. The state shall review the recommendations and authorize new capital expenditures; any capital improvement project shall be administered by the health care organization.
c. Basic health care services provided by the health care organization shall include yearly physicals (provided at no charge), infant and childcare (routine checkups to be provided free of charge), typical sicknesses (such as flu or sinus infections), minor injuries (such as sprained ankles or minor fractures), and basic diagnostics (X-rays, MRIs, CAT-scans, blood analyses, colonoscopies, mammograms, and other routine diagnostics). Maternity services are provided, including childbirth facilities, except that C-sections or other difficult births will be handled by affiliated hospitals. For each visit that is not provided free of charge, there will be a minimal copay requirement (e.g. $20).
d. For emergencies and surgical procedures, individuals covered by the state will have access to hospital emergency facilities. For any work done by the hospital, the hospital shall be reimbursed by the state, but only for the time and materials that are used for the procedure – only the hourly wages of staff involved in the procedure and the actual materials used will be reimbursed.
Now, more on HSAs. The goal of HSAs is to allow people to contribute to and grow a fund that will be available to use when they retire. Contributions to the HSAs can also be used to purchase health insurance and to pay for surprise medical costs due to an injury or illness. While these latter two uses for an HSA are important, these uses should be somewhat constricted, as the primary point of the HSAs is to build up a nest egg for health insurance upon retirement. Here is a summary of key features of HSAs:
Just like 401k retirement plans, HSAs will be tax-free contributions, and the funds will be invested in plans that will involve stocks and bonds with an expectation of growth similar to the stock market’s growth. Each person will have control over their HSA fund, including making decisions regarding the plans the contributions will be made to and transferring funds from one plan to another.
The funds cannot be used for anything other than health costs. Upon death, a person’s HSA can be passed on to spouses, children, friends, or to charitable organizations (such as the Shriner’s hospital) that provide health care or assist individuals with unexpected health care costs. No taxes shall be leveled upon death.
Currently, Medicare taxes are levied at a rate of 1.45 percent of a person’s wages. Employers contribute an equal amount, resulting in a total tax of 2.9 percent. With the proposed HSA approach, employees and employers must contribute the same amount to an HSA fund. Individuals can contribute more than this minimum with no limit. Someone making $20 per hour and working full-time, will contribute $600 per year to his HSA, and his employer will contribute an equal amount, giving a total of $1,200.
Up to half of the yearly contribution to the HSA can be spent to purchase insurance or pay for medical expenses. This amount is carried over to subsequent years if it is not spent. For example, if the total contribution is $1,200 in a year, $600 could be used for insurance or medical expenses. If only $100 of this amount is used, the remaining $500 is carried over and could be used in later years.
HSA contributions become vested two years after the contribution is made. Once vested, the funds cannot be taken by others for medical costs. Non-vested funds, on the other hand, can be garnished by health care organizations that are seeking payment for medical expenses, in the event of an individual not paying for medical services received. If garnishment is used, the amount taken per month shall be limited to the 25 percent of the total contribution by both the employee and employer. An example of garnishment is as follows:
a. A person owes $2,000 in medical expenses and has either exhausted his available HSA funds or refuses to pay the expenses.
b. He and his employee contribute $200 per month to the HSA. The health care organization that is owed $2,000 submits the costs to the State health care organization for their review and approval of garnishment. They notify the person who owes the $2,000 that they are reviewing a garnishment request and allow the person to provide his input, if any. After approval of garnishment, the State initiates the garnishment process, which in this example, will divert $50 per month to the health care organization. A low interest rate charge is also applied (perhaps tied to the current Federal interest rate plus one percent). Assuming the person’s monthly pay remains the same, the $2,000 would be paid off in 40 months with a few additional months required to pay off the interest.
c. The person who owes the $2,000 can pay off the remainder of the expense at any time to stop garnishment.
Based on an individual’s circumstance, there are several possibilities that can occur with the proposed approach that merit further discussion. I will cover some is this Paper, but undoubtedly there are other situations that should be discussed and examined before the proposed approach is finalized. The intent of this Paper is to put forward the main features of the proposed plan with the understanding that the details of the plan will need to be thoroughly vetted.
Individuals that are provided insurance as a benefit from employment are covered and secure. Individuals that do not get insurance from their employer include the following (with discussion of how these individuals would most likely address their health insurance):
Self-employed. These individuals will also be required to establish an HSA and make contributions to it based on their income and/or the profits of the business they own. Some self-employed individuals could qualify for the low-income health care provided by the states, but most will likely be able to afford insurance.
Low-income, but employed. These individuals would qualify for low-income health care provided by the state or could elect to purchase insurance on their own. By purchasing their own insurance, they would have more choice than if they relied on the state health care.
Employed, with an income that is too high to qualify for state health care. Some of these individuals (such as young healthy single persons) may choose to go without insurance. If they do not have insurance and have an accident of severe illness, should these individuals be allowed to purchase insurance after-the-fact? This case can be addressed by having a delay (such as thirty days) in the time from when insurance is purchased until it becomes usable. With this approach, the individual who has an injury or illness will be responsible for all medical costs for at least thirty days. For example, assume an individual becomes ill and goes to the doctor for a diagnosis. The doctor orders tests, which would be paid for by the patient, and the test results indicate the patient has lung cancer. The patient then purchases insurance and delays treatment until the insurance becomes usable. In this case, the patient would be placed in the insurance pool for individuals with preexisting conditions – the cost of the insurance is the same as anyone else, but the patient is assigned an insurance company. In addition to delaying the start of insurance, anyone that purchases insurance will be required to pay for the insurance for at least one year.
Unemployed and not physically or mentally disabled. For someone that was employed, got insurance from his employer, and lost his job, he can continue to pay for insurance by taking over the payments. In this case, the insurance company shall be required to offer lower cost plans if the employer’s insurance was a low deductible plan. For someone that is able-bodied and could find a job but is chronically unemployed because of poor behavior on the job (resulting in getting fired) and/or laziness, he can apply for the state low-income health care. Most of these individuals will be approved for this health care; however, as part of receiving the health care, they will be required to attend job counseling, with the goal of helping them learn to find and keep jobs. If they do not attend the counseling sessions, their state health care card will be cancelled. In this case, their only avenue for health care is to go to the hospital emergency room whenever they have a severe medical condition.
Physically or mentally disabled and unemployable. Ideally, a physically or mentally disabled person will be able to find employment. If they are unable to find employment, they have many concerns regarding how they live, including the basics of life – housing, food, transportation, and others, as well as health care. As such, I will address how the government can help these individuals in another American Rebirth Paper.
Addicted to drugs and/or alcohol and unemployable. Some addicts and alcoholics can stay employed, but many are not because their addictive behavior is a 24/7 situation. Besides their addiction, these individuals also may have mental issues and often are homeless. Obviously, their health issues are a problem. Hospital emergency rooms are the best method to deal with health issues, such as overdoses, that occur when these individuals interact with law enforcement officers or social workers because of a health problem. Long term, helping these individuals give up drugs and alcohol should be the goal; how we can best provide help will be addressed in another American Rebirth Paper.
Seniors that exhaust their HSA funds and have no other means to pay for health care. These individuals will need to apply to the state for health care benefits. In addition to the states providing health care to low-income individuals, the states shall also operate low-income facilities that can provide assisted living and memory care for elderly individuals. As with the health care facilities, the assisted living/memory care facilities shall be owned or leased by the state, but operated by a private health care organization, which is contracted to the state after a competitive bidding process. A third-party organization, also contracted to the state, shall provide oversight of the private health care organization, including inspections and user surveys, to gauge the health care organization’s performance against the contract.
Now that I’ve described a new approach to health care that eliminates Federal government funding, I will now discuss how we can transition from the current Medicare program to an HSA program. As discussed in American Rebirth Paper No. 7, the Social Security program is essentially a Ponzi scheme that relies on new investors (in this case taxpayers) to support benefits to old investors. The Medicare program is also a Ponzi scheme, and as with all Ponzi schemes, when the finances of the scheme are no longer sustainable, some investors in the scheme will lose. In eliminating Medicare, therefore, the best approach is to phase out the program to even out the loses across as many investors as practical. My suggested approach is as follows:
Individuals that are over 65 and are currently using Medicare will be covered as they are now until they die.
Individuals under the age of 65 who are covered by Medicare for health issues will be covered by the state health care programs and/or disability program.
Individuals that are under 40 years old will not qualify for Medicare.
Individuals that are 40 to 65 years old will get one year of Medicare coverage for each year over 40. For example, someone that is 45 years old will get 5 years of Medicare coverage starting when they are 65 years old. With this approach, most of the Medicare program will be phased out in 25 years. Since some individuals who are currently getting Medicare may live for more than 25 years, there will be additional years where the Medicare program will still need funding.
Required funding for Medicare during the transition period will be provided by a national sales tax and/or a value-added tax. In addition, a small tax (perhaps 0.1%) will be assessed on all financial transactions.
The Medicaid program is currently administered by the states with some of the cost provided by the Federal Government. With the proposed program described herein, the states will continue to administer health care programs for low-income individuals and funding for these programs will be entirely covered by each state for their respective programs. Only one or two years will likely be required to make this transition.